1.In case of death in lock up, the inquest is held by –
a) A Police officer b) Magistrate (PGI 86)
c) Panchayat officer d) District Attorney
2.In India, inquest is carried out by all except –
a) Police b) Coroner (AIIMS 91)
c) Doctor d) Magistrate
3.The enquiry into the circumstances of death is
called – (TN 91)
a) Homicide enquiry b) Inquest report
c) Open verdict d) Adjounred verdict
4.The common type of inquest in India is –
a) Coroner’s inquest – (Karn 94)
b) Police inquest
c) Judicial magistrate inquest
d) Medical examiner’s inquest
5.In India, magrstrate inquest is done in the following
cases except – (A1 05)
a) Exhumation cases
b) Dowry deaths within 5 years of marriage
c) Murder cases
d) Death of a person in police custody
U/S 174 Cr.P.C-Police to enquire -Under section 174(subsection 3) Cr.P.C, it’s mandatory provision which requires that the body of a woman, who has committed suicide within seven years of her marriage, has to be subjected to postmortem examination and the inquest also has to be held.
U/S 176 Cr.P.C.-Inquiry by Magistrate into cause of death:-[When any person dies while in the custody of the police or when the case is of the nature referred to in clause (i) o or clause (ii) of sub-section (3) of section 174] the nearest Magistrate empowered to hold inquests shall, and in any other case mentioned in sub-section (1) of section 174, any Magistrate so empowered may hold an inquiry into the cause of death either instead of, or in additional to, the investigation held by the police officer; and if he does so, he shall have all the powers in conducting it which he would have in holding an inquiry into an offence.
Magistrate’s inquest means an inquiry conducted by a magistrate to ascertain matters of fact. It is commonly held in the following cases: Admission of a mentally ill person in a psychiatric hospital or a psychiatric nursing home under certain provisions of the Mental Health Act, 1987; Death of a convict in jail; Death of a person in police custody or during police interrogation; Death as a result of police shooting killing; Exhumation cases and Dowry deaths under section Sec 176 Criminal Procedure Code, 1973.
Important Crpc Sections:-
193 crpc–Perjury means giving willful false evidence by a witness while under oath, the witness is liable to be prosecuted for perjury and the imprisonment may extend to seven years. This falls under 193 of Penal Code
Section 53:- Examination at the request of police
Section 54:- Examination at the request of accused (imp:-NOT victim)
IPCs:-
44-Injury Body Mind Reputation Property
84-Criminal responsibility of insane
85-Involuntary Drunkeness
86-Voluntary Drunkensess
312-316 Deals with criminal abortion
317- Abandoning of child by parents
318- Concealment of death of infant
definition of rape is sec 375
punishment for rape is sec 376
sec 377 is about unnatural sexual offences
Sections 354 (molestation),Section 354 of the IPC considers the assault or criminal force to woman with the intention to outrage her modesty. This offense is considered less serious than Rape.
Section 509. Word, gesture or act intended to insult the modesty of a woman.– Whoever, intending to insult the modesty of any woman, utters any word, makes any sound or gesture, or exhibits any object, intending that such word or sound shall be heard, or that such gesture or object shall be seen, by such woman, or intrudes upon the privacy of such woman, shall be punished with simple imprisonment for a term which may extend to one year, or with fine, or with both.
506 (2) (criminal intimidation)
The India Penal Code 1860 does not recognise child abuse. Only rape and sodomy can lead to criminal conviction
Section 5 of the Immoral Traffic Prevention Act 1956 prescribes punishment of not less than 7 years for inducing a child into prostitution, but does not directly address child abuse.
Most of these forms of child abuse are sought to be covered under sec. 354 of the Indian Penal Code as a violation of a woman’s modesty. Though offences under Sec. 354 of the IPC are cognizable, they are also bailable, allowing the perpetrator to abscond before the case comes up in court.
300-Defines MURDER
299-Defines CUL. HOMIICIDE NOT AMOUNTIN TO MURDER
Section 302. Punishment for murder
Section 304:- Punishment for 299
Section 304. Punishment for culpable homicide not amounting to murder
Whoever commits culpable homicide not amounting to murder shall be punished with 1 [imprisonment for life ],or imprisonment of either description for a term which may extend to ten years, and shall also be liable to fine, if the act by which the death is caused is done with the intention of causing death, or of causing such bodily injury as is likely to cause death,Or with imprisonment of either description for a term which may extend to ten years, or with fine, or with both, if the act is done with the knowledge that it is likely to cause death ,but without any intention to cause death, or to cause such bodily injury as is likely to cause death
Sec 304 A Death due to negligent act (Medical or any)-2yrs punishment:-
Section 304A. Causing death by negligence
1[304A. Causing death by negligence.
Whoever causes the death of any person by doing any rash or negligent act not amounting to culpable homicide, shall be punished with imprisonment of either description for a term which may extend to two years, or with fine, or with both.]
Medical negligence falls under section 304A
Sec 304 b is dowry death- 7 yrs to Life imprisonment
Section 320. Grievous hurt.
Section 312. Causing miscarriage
Section 37. Co-operation by doing one of several acts constituting an offence–A and B agree to murder Z by severally and at different times giving him small doses of poison. A and B administer the poison according to the agreement with intent to murder Z. Z dies from the effects of the several doses of poison so administered to him. Here A and B intentionally co-operates in the commission of murder and as each of them does an act by which the death is caused, they are both guilty of the offence though their acts are separate.
IPC Crimes
(i) Procuration of minor girls (section 366-A IPC)
(ii) Importation of girls ((Sec. 366-B IPC)
SLL Crimes
(i) Immoral Trafficking (Prevention) Act 1956
(ii) Child Marriage Restraint Act, 1929.
Section 366B. Importation of girl from foreign country
1[366B. Importation of girl from foreign country. Whoever imports into 2[India] from any country outside India 3[or from the State of Jammu and Kashmir] any girl under the age of twenty-one years with intent that she may be, or knowing it to be likely that she will be, forced or seduced to illicit intercourse with another person, 4[***] shall be punishable with imprisonment which may extend to ten years and shall also be liable to fine.]
Section 366A. Procreation of minor girl
1[366A. procreation of minor girl.:–Whoever, by any means whatsoever, induces any minor girl under the age of eighteen years to go from any place or to do any act with intent that such girl may be, or knowing that it is likely that she will be, forced or seduced to illicit intercourse with another person shall be punishable with imprisonment which may extend to ten years, and shall also be liable to fine.]
Section 372. Selling minor for purposes of prostitution, etc
Section 373. Buying minor for purposes of prostitution, etc.
Section 299. Culpable homicide
Who ever causes death by doing an act with the intention of causing death, or with the intention of causing such bodily injury as is likely to cause death, or with the knowledge that he is likely by such act to cause death, commits the offence of culpable homicide.
Section 300. Murder
Except in the cases hereinafter excepted, culpable homicide is murder, if the act by which the death is caused is done with the intention of causing death, or-2ndly If it is done with the intention of causing such bodily injury as the offender knows to be likely to cause the death of the person to whom the harm is caused, or-3rdly If it is done with the intention of causing bodily injury to any person and the bodily injury intended to be inflicted is sufficient in the ordinary course of nature to cause death, or-4thly If the person committing the act knows that it is so imminently dangerous that it must, in all probability, cause death or such bodily injury as is likely to cause death, and commits such act without any excuse for incurring the risk of causing death or such injury as aforesaid.
Illustrations
(a) A shoots Z with the intention of killing him. Z dies in consequence. A commits murder.
(b) A, knowing that Z is labouring under such a disease that a blow is likely to cause his death, strikes him with the intention of causing bodily injury. Z dies in consequence of the blow. A is guilty of murder, although the blow might not have been sufficient in the ordinary course of nature to cause the death of a person in a sound state of health. But if A, not knowing that Z is labouring under any disease, gives him such a blow as would not in the ordinary course of nature kill a person in a sound state of heath, here A, although he may intend to cause bodily injury, is not guilty of murder, if he d8id not intend to cause death, or such bodily injury as in the ordinary course of nature would cause death.
(c) A intentionally gives Z a sword-cut or club-wound sufficient to cause the death of a man in the ordinary course of nature. Z dies in consequence. Here, A is guilty of murder, although he may not have intended to cause Z’s death.
(d) A without any excuse fires a loaded connon into a crowd of persons and kills one of them. A is guilty of murder, although he may not have had a premeditated design to kill any particular individual.
Exception I-When culpable homicide is not murder-Culpable homicide is not murder if the offender, whilst deprived of the power of self-control by grave and sudden provocation, causes the death of the person who gave the provocation or causes the death of any other person by mistake or accident.
The above exception is subject to the following provisos :–
First-That the provocations not sought or voluntarily provoked by the offender as an excuse for killing or doing harm to any person.
Secondly-That the provocation is not given by anything done in obedience to the law, or by a public servant in the lawful exercise of the powers of such public servant.
Thirdly-That the provocations not given by anything done in the lawful exercise of the right of private defence.
Explanation-Whether the provocation was grave and sudden enough to prevent the offence from amounting to murder is a question of fact.
Culpable Homicide not Amounting to Murder is an offence under s.304 of the Indian Penal Code. It applies to an event where the death is intentional but does not come within the IPC definition of Murder.
Murder versus Culpable Homicide:
Murder (defined under Section 300) and culpable homicide (defined under Section 299) are two offences under the Indian Penal Code the distinction between which has always been perplexing to the law students.
Section 299 and Section 300 IPC deals with the definition of culpable homicide and murder respectively. Section 299 defines culpable homicide as the act of causing death; (i) with the intention of causing death or (ii) with the intention of causing such bodily injury as is likely to cause death or (iii) with the knowledge that such act is likely to cause death. The bare reading of the section makes it crystal clear that the first and the second clause of the section refer to intention apart from the knowledge and the third clause refers to knowledge alone and not intention. Both the expression “intent” and “knowledge” postulate the existence of a positive mental attitude which is of different degrees. The mental element in culpable homicide i.e. mental attitude towards the consequences of conduct is one of intention and knowledge. If that is caused in any of the aforesaid three circumstances, the offence of culpable homicide is said to have been committed. Section 300 IPC, however, deals with murder although there is no clear definition of murder provided in Section 300 IPC. It has been repeatedly held by this Court that culpable homicide is the genus and murder is species and that all murders are culpable homicide but not vice versa. Section 300 IPC further provides for the exceptions which will constitute culpable homicide not amounting to murder and punishable under Section 304. When and if there is intent and knowledge then the same would be a case of Section 304 Part I and if it is only a case of knowledge and not the intention to cause murder and bodily injury, then the same would be a case of Section 304 Part II. The aforesaid distinction between an act amounting to murder and an act not amounting to murder has been brought out in the numerous decisions.
————(a) 300 (amounting to murder).Definition
Section 299(culpable homicide)
————b) 304 (not amounting to murder).Punishment for 299 if not (a)
_______c) 302 Punishment if (a)
Which carries more weight in a court of law –
a) Dying declaration (PGI 87)
b) Dying deposition
c) Both carry the-same weight
d) Both are not significant
Dying declaration is very important documentary evidence. It is hearsay evidence but even then it is given a lot of weightage in the court proceedings. Recording of dying declaration is very important. If it is recorded properly by the proper person keeping in mind the essential ingredients of the dying declaration it retains its full value. Missing any single ingredients of dying declaration makes it suspicious and offenders are likely to get the benefits of its shortcomings.
Its admissibility is explained in the section 32 (1) of Indian Evidence Act. According to this section when the statement is made by a person as to the cause of his death, or any of the circumstances of the transaction which resulted in his death, in cases in which the cause of that person’s death comes into question. Such statements are relevant whether the person who made this was expecting death or not [1]. In English law he must be under expectation of death only then this declaration is valid.
This can be best certified by the doctor who knows best about the condition of the patient. But even in conditions where it was not possible to take fitness from the doctor, dying declarations have retained their full sanctity if there are other witnesses to testify that victim was in such a condition of the mind which did not prevent him from making statement. Medical opinion cannot wipe out the direct testimony of the eyewitness stating that the deceased was in fit and conscious state to make the dying declaration.
It is best that it is recorded by the magistrate but if there is no time to call the magistrate due to the deteriorating condition of the victim it can be recorded by anybody e.g. public servant like doctor or any other person. Courts discourage the recording of dying declaration by the police officers but if there is no body else to record it dying declarations written by the police officers are also considered by the courts. If these are not recorded by the magistrate it is better that signatures of the witnesses are taken who are present at the time of recording it.
Ideally it should be recorded by executive magistrate. [But if magistrate is not available, it can be recorded by doctor himself or if the patient is not in the hospital it can also be recorded by any person present near the patient.] Doctor has to certify pt.to be ‘compos mentis’ .During recording police, relatives should not be present there. .It should be recorded in the presence of magistrate, doctor & 2 disinterested witness. .No oath is administered & leading questions are not permitted. .It is recorded in Question & answer form in the vernacular of patient.
At the end it is read over to the patient & is signed by the magistrate, doctor & 2 disinterested witness. If the patient dies during recording Dr. should certify that pt. is dead & incomplete declaration is signed by all the concerned. The date, time & place of recording is noted & report is sent to magistrate (if not present) in a sealed cover. If the pt. survives after recording, the declaration looses its value, because now he can be called to the court for evidence where cross examination will be possible.However under section 157 IEA,the declaration may still be relied upon to corroborate the statement of the complainant at the time of oral examination.
Ref:-JIAFM, 2004; 26(1). ISSN 0971-0973
CRITICAL APPRAISAL OF DYING DECLARATION
Dr. R.K.Gorea, Professor and Head, Forensic Medicine, GMC, Patiala
Dr. O.P.Aggarwal, Professor, Forensic Medicine, M.M. Medical College, Mullana, Ambala
DYING DEPOSITION It is defined as the deposition (statement on oath) made by a person likely to die bcoz of some unnatural act done on his body,narrating the cause of his likely unnatural death to the magistrate, in the +nse of accused & lawyers of both parties who can cross examine the pt. Precautions- It should by magistrate, in the +nse of accused & lawyers of both parties. Dr. has to be +ntthrough out the procedure & has to certify the pt. in compos mentis. Oath is administered to the pt. Cross examination includes leading questions.Any person may be present during recording .No witness required. Recording is done as per the procedure of court & hence almost it seems that a court is +nt at bedside of pt.
Importance-Dying deposition is having more value than that of dying declaration bcoz, It is recorded by magistrate. In the +nseof accused & lawyers of both parties. It is recorded after cross examination. It retains its value even if pt. survives bcozcross examination has already been done.
The power of Amnesty for capital punishment
is vested with – . (AMU 88)
a) The president b) Supreme court
c) High court d) The governer
Amnesty is a legislative or executive act by which a state restores those who may have been guilty of an offense against it to the positions of innocent people. It includes more than pardon, in as much as it obliterates all legal remembrance of the offense.
Courts can only give stay order pending hearing for a lower court order.
Conduct money is paid to expert witness with
summons from – (AI 90)
a) Civil court b) Criminal court
c) High court d) Sub magistrate
Conduct money is the money paid by the court of law to the witness who is under summon or subpoena to meet his travelling expenses from his place of residence to the court, and back . In CIVIL cases , this is paid to witness at the time the summon is served on him . If this amount is not paid to him/her, he/she may ignore the summons, if he/she so desire. If he/she feels the sum is inadequate can inform the court accordingly & get it enhanced . In CRIMINAL cases however, no such fee is given usually, & it is bounden duty of every citizen to attend the court whenever summoned.(It may however be noted that provision is made by government under section 312 of Crpc for payment of reasonable expenses of an expert witness attending before any criminal court.Payment of reasonable expenses of an expert witness in magistrate courts in summons cases is provided for under section 254(3) and in warrant cases under section 243 (3) CrPC.)
Death sentence can be awarded by – (Kerala 91)
a) First class magistrate
b) Second class magistrate
c) Session court
d) Chief judicial magistrate
Important POINTS:-
1.A session court cannot commute death sentence.How can it commute a death sentence when it is the lowest court to announce the death sentence.
2.President cant Give death sentence It can give amnesty/mercy plea.
3.Additional session court have same power as session court
4.Assistant session court has lower power.
5.None of the magistrate can give death sentence or Life imprisonment
6.CJM power:- 7 years,fine without limit
1st class Judicial magistrate power:- 3 years,upto Rs 5000
2nd class Jud Mag:- 1 Year Max, upto 1000
- According to Indian Majority Act 1875, a person attains majority when he/she attains the age of 18 years.
- According to Section 4(a) of the TheHindu Minority and Guardianship Act 1956, a person who is below 18 years of age is a minor.
Age
According to Section 363-A of I.P.C, kidnapping or maiming of a minor for the purpose of begging is an offence. If the person merely kidnaps, the sentence is 10 years and fine. If he maims, the sentence is life imprisonment and fine. For the purposes of this section a minor is a female below 18 years (or a male below the age of 16 years). This is an interesting section, as the ages for minors are different for males and females.
However Sections 87 IPC mentions eighteen years as the age for giving consent for acts not intended and not known to be likely to cause death or grievous hurt. These acts are not necessarily for the benefit of the person . Hence Section 87 IPC is not applicable to the medical profession as here (in Section 87 IPC), the acts are NOT done for the person’s benefit. .
According to Section 87 of I.P.C, a person under the age of 18 years can not give valid consent whether express or implied to suffer any harm which may result from an act not intended or not known to cause death or grievous hurt (example: fencing)’
According to Section 89 of I.P.C, a child below 12 years can not give valid consent to suffer any harm which may occur from an act done in good faith and for its benefit(as a general physical examination by a doctor,surgical operations).
The age of a 16 years old female is best determined
by the radiograph of – (PGI 87)
a) Lower end of radius and Ulna
b) Upper end of humerus
c) Upper end of radius and Ulna
d) Xiphisternum
Female Male
Elbow 13-14 yrs 15-17 yrs
Wrist:- 16-17 years 18-19 yrs
Shoulder 17-18 19-20 yrs
Crest of Ilium 18-19 20-21yrs
Ref Parikh
Elbow(13-14)—Wrist(16-17)—Shoulder(17-18)—Crest of ilium(18-19) Add plus 2 for Males
By 13-14 years the epiphysis at the elbow join their respective shafts in Females. In males by 16-18 yrs.,all the epiphysis at the elbow (except the medial epicondyle),head of the femur,and lower end of tibia join the respective shafts.
The age of a 15 year old female is best determined
by the radiograph of –
a) Lower end of Radius and Ulna
b) Upper end of humerus
c) Upper end of Radius and Ulna??? NOT SURE
d) Xiphisternum
Ossification centre appearing just before birth is—LOWER END OF FEMUR
Capitate and hamate ossify at the age of 4 months,so before 4 months of age,no bone is seen on radiography
Pre-auricular sulcus is used for – (AMJ 88)
a) Determination of Race
b) Determination of age
c) Determination of sex
d) None of the above
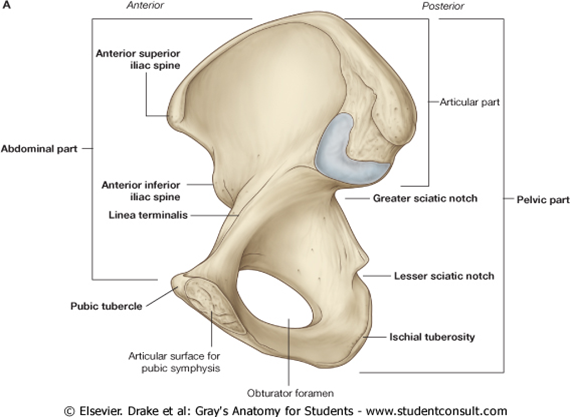
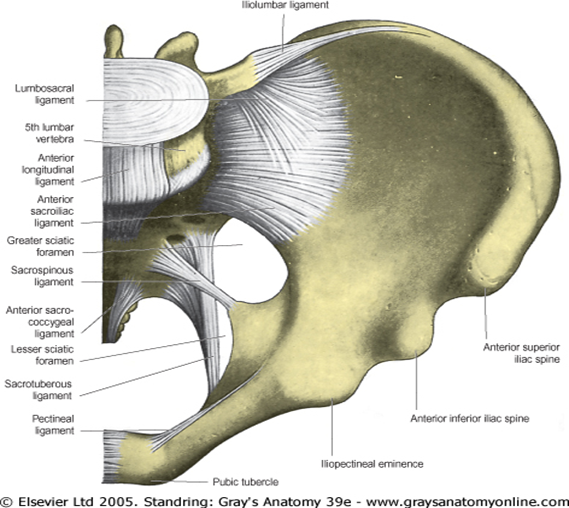
The narrow part of the pelvic surface, between the auricular surface and the upper rim of the greater sciatic notch, often shows a rough preauricular sulcus for the lower fibers of the anterior sacroiliac ligament, more apparent in females.
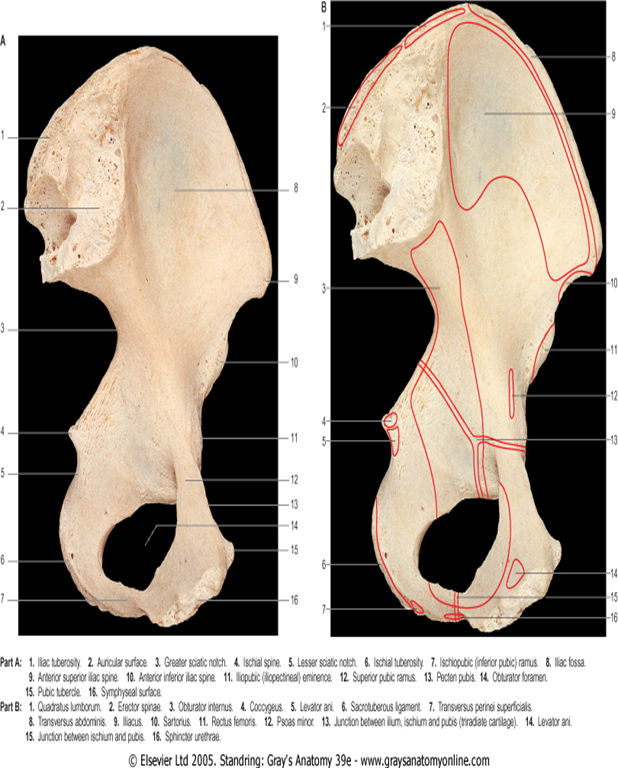
In forensic practice, identification of human skeletal remains (which are sometimes fragmentary) usually involves diagnosis of sex, and this is most certainly established from the pelvis. Even parts of the pelvis may be useful. Several studies of metrical characteristics in various pelvic regions have been made, leading to the production of various indices. The ilium has received particular attention, e.g. one index compares the pelvic and sacroiliac parts of the bone. A line is extended back from the iliopectineal eminence to the nearest point on the anterior auricular margin and thence to the iliac crest. The auricular point divides this chilotic line into anterior (pelvic) and posterior (sacral) segments, each expressed as a percentage of the other. Chilotic indices display reciprocal values in the sexes: the pelvic part of the chilotic line is predominant in females, and the sacral part in males. Detailed metrical studies of the ilium have indicated its limited reliability in ‘sexing’ pelvis. However, the higher incidence and definition of the female preauricular sulcus is recognized.The desirability of correlating all available metrical data is to be emphasized; when a range of pelvic data can be combined, especially if they are metrical, 95% accuracy should be achieved. Complete accuracy has been claimed when the rest of the skeleton is available. Assessment of sex from isolated and often incomplete human remains is less reliable.
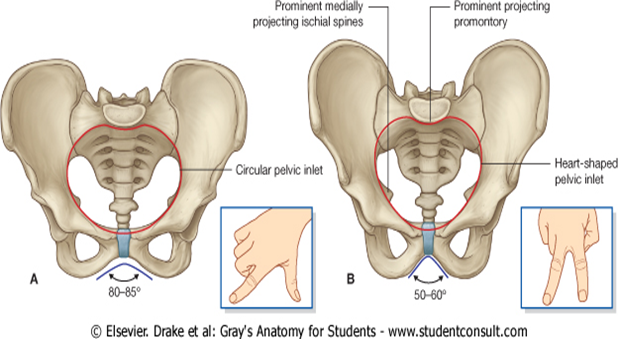
Males:-Suprapubic arch narrow,V shaped,angle not more than about 70 degrees and hence less Distance between ischia,Greater sciatic notch is narrow,deep,and less than right angle.Obturator foramina ovoid.Ischial Tuberosities inverted
Females:- Suprapubic arch wide,U shaped,angle more than a right angle and hence more distance between ischia.Greater sciatic notch is wide shallow and almost a right angle or more.Obturator foramina triangular.Ischial Tuberosity everted.
Structure of the bony pelvis. A. In women. B. In men. The angle formed by the pubic arch can be approximated by the angle between the thumb and index finger for women and the angle between the index finger and middle finger for men as shown in the insets.
Skull:- Orbital opening big and rectangular in males while it is rounded and small in females.Muscle attachments are more pronounced in males.
Cephalic index(for the determination of race) is obtained by multiplying the maximum transverse breadth by 100 and dividing it by maximum AP Length. A skull is dolichocephalic(long headed)—70-74.9 seen in Aryans,aborigines,and blacks.
Mesaticephalic is medium long headed—75—79.9—seen in European,, Indians and Chinese.
Mongolian- is Brachycephalic——index is more than 80or above..(transverse diameter approaches 80 per of AP length).
100 % sex differentiation is not possible by pelvis alone.Entire skeleton is needed.
According to Krogman:- Pelvis alone—95%
Skull alone—90%
Long bones alone—80%
Pelvis and Skull—98%, Entire skeleton—100%
A method of sexing of bones by the use of medullary index has also been described.The humerus,radius,ulna,and tibia are the most reliable bones for this purpose.
Medullary index:- Diameter of medulla/diameter of whole bone multiply by 100
There is thinning of cortex in old age so it may also give some idea about age.
Medullary index of Hair is used to distinguish between animal or human hair.In animals it is more than 0.5 while in humans it is less than 0.3.
In human hair,only the cortex is pigmented;the medulla is narrow ,absent or pigmented.In Negros’s fragmentation of medulla of scalp hair is seen.
Teeth:-
Temporary—Lower central incisors,2(6-8 months)—-Upper central incisors,2(7-9 months)———Upper Lateral incisors,2(7-9 months)———Lower lateral incisors,2(10-12 months)——-First molars,4(12-14 months)———Canines,4(17-18 months)——-Second Molars,4(20-30 months)
Permanent—-First Molars,4(6-7 years)—At new place
Central incisors,4(6-8 years)—Replacement
Lateral incisors,4(8-9 years)—Replacement
First bicuspids/premolars,4(9-11 years)—-Replaces 1st temp molar
Second bicuspids/premolars,4(10-12 years)-Replaces second temp molars
Canines,4(11-12 years)—-Replaces temp canines
Second molars,4(12-14 years)—-At new place
Third Molars,4(17-21 years)—— At new place
All permanent molars are additions at new place not replacements behind the second temporary molars.
There is no temporary premolars or bicuspids.Only permanent.
Premolars replaces first and second temporary molars.
The best method to determine age up to 14 years is DENTITION.
20-Temporary teeths-TEMP DENTITION COMPLETES AT ABOUT 2 AND HALF YEARS
The temporary teeth begin to shed from the 6th to 7th years after the eruption of first molar behind the second “temporary” molar teeth and all temporary teeths have shed when permanent canines appears.Period of mixed dentition is from 6-11 years.
MOST IMPORTANT POINT:-From the age of 6 years till the age of 12 years-The total number of teeth remains 24 in number as 4 permanent molars in 6 years are added at new place other permanent teeth’s replaces temporary teeths; so total number doesn’t changes after addition of first permanent molars till the appearance of second molars at the age of 12-14 years.
A girl of 10 years will have 24 teeth—16 permanent and 8 temporary teeths
TEMP TEETH APPEARANCE-MIB CM—-MOLAR INCISORS BICUSPIDS CANINES MOLARS
M -7 yrs—-NEW PLACE
I —CENTRAL—8yrs LATERAL—9yrs—REPLACEMENT
B -BICUSPIDS—FIRST—10yrs SECOND—11yrs—REPLACEMENT
C —CANINES—12yrs—REPLACEMENT
M OLARS—SEC—12-14 YRS, WISDOM/THIRD—17-21 YEARS—NEW PLACE
FIRST PERMANENT MOLARS AT 6 YEARS,SECOND AT 12 YRS.
MOLARS ARE TRICUSPIDS.
Q:-Second molar erupts at – (A1 91)
a) 6 years b) 12 years
c) 18 to 22 years d) 25 to 28 years
20 permanent teeth and 8 temporary teeth are
seen at the age of – (Kerala 2001)
a)10yrs b) 11 yrs
c) 9 v s dl 12 yrs
First permanent tooth to arise- (JIPMER 02)
a) Incisor b) Canine
c) Premolar d) Molar
Among the secondary changes in tooth the most
useful one for age determination is – (Corned 08)
a) Attrition
b) Secondary dentine deposition
c) Root resorption
d) Root transparency
On tenth day of a tooth being knocked out, the local
clinical finding will be – (AIIMS 81, Kerala 89)
a) Tooth socket being filled up by tissue
b) Blood clots in the socket
c) Alvoelar process smooth
d) Fluid blood in the socket
In antemortem tooth loss or extraction of the
alveolus is – (Karnataka 02)
a) Smooth
b) Sharp and feathered
c) Does not show any injury
d) sMay have a regular or an irregular appearance
When a tooth has been knocked out,bleeding from its socket stops in about one to two days and a clot is formed.The clot is obliterated by fibrous tissue in about 14 days.The socket is completely filled with gradual new bone in about a year,as seen on X-RAY examination.
Eruption of temporary teeth will be completed by
a)One to one and half year (JIPMER 81,
b) Two to two and half years Kerala 90)
c) Three to four years
d) Four to five years
A girl of 10 years wilt have —- permanent and
–temporary teeth – (PGI 79, DNB 90)
a) 8,12 b)8,16
c) 12,12 d) 16,8
A child at the age of 7 years has how many teetha)
16 b) 20 (PGI 83, UPSC 81)
C) 24 d) 28
IMPORTANT:- A boy has 20 permanent and 8 temporary teeth
his age would be – ‘ (APPPGE 04)
a) 9 years b) 10 years
c) 11 years d) 12 years
Answer in guides is 10 years.But answer is d i.e.12 years.
The total number of teeths is 28 in this Q
“In question there should have been 16 permanent and 8 temp teeth.If there are 20 permanent teeth there should be 4 temp teeth. But since there is total number of 28 teeth,A second molars must have got erupted also so age must be 12 years.8 temporary teeth i.e canines and second temp molars also get replaced as late as 12 years.So period of mixed dentition persists till about 12 to 13 years.The bicuspids are most irregular and are of little value in fixing age.”
8 TEMP TEETH are still here so 4 temporary canines and 4 temporary second molars are not replaced by 4 permanent canines and 4 permanent second premolars respectively but 4 second permanent molars have got erupted at new place making total number to 28 .since 24 teeth are till 12 years of age only. so age is 12 years.
B -BICUSPIDS—FIRST—10yrs SECOND—11yrs—REPLACEMENT
C —CANINES—12yrs—REPLACEMENT
Number of deciduous teeth is – (JIPMER 95)
a) 20 b) 24
C) 28 d) 32
Tattoo is useful in identifying body – (A1 91)
a) Living b) Dead
c) Decomposed d) Burnt
Tattoo marks on unidentified putrefied bodies may be photographed with a sharp definition if the loose epidermis is first removed and the design on the dermis recorded.
Blackening and tattooing of skin and clothing can
be best demonstrated by – (A1 03)
a) LuminoI spray
b) Infra red photography
c) Ultra violet light
d) Magnifying lens
To reveal latent tattoo marks,the use of high-contrast photography,computer image enhancement,ultraviolet lamp or infra-red photography is helpful.
Tattooing is seen surrounding the wound of
entrance from a revolver or pistol, if the weapon
is discharged up to distance of – (COMEDK 05)
a) 10 cm b) 30 cm
c) 50 cm d) 90 cm
Rigor mortis
Rigor mortis is simulated by – (AIIMS 92)
a) Mummification b) Algor mortis
c) Cadaveric spasm d) All of the above
Stiffening and shortening of muscles.
After death ATP is resynthesized for a short period of time depending upon the glycogen available locally,but after this glycogen is used up,ATP cannot be resynthesized.This leads to fusion of myosin and actin filaments into a dehydrated stiff gel resulting in condition known as RIGOR MORTIS.
imp-it is due to decreased ATP not due to increase.
It can be broken down by mechanical force.
In the involuntary muscles,rigor mortis appear in the heart within an hour after death.
In the voluntary muscles sequence is as follows:-
EYELIDS(3-4 HRS)—->FACE(4-5 HRS)—->NECK AND TRUNK—->(5-7 HRS)——>MUSCLES OF UPPER EXTREMITIES—->(7-9 HRS),—-> of the legs(9-11hrs)—–>FINGERS AND TOES(11-12 HRS)
In india rigor mortis commences within 2-3 hrs,takes about 12 hrs to develop from head to toes,persist for another 12 hrs and takes about 12 hrs to pass off.
So if rigor mortis has not set in,the time since death would be within 2 hours and if it has affected the whole body,the time since death would be within about 12- 24 hrs.
Rigor mortis in fetus develops after attaining 7 months of age.
As a general rule,the longer it takes to appear for rigor,the longer it lasts and vive versa.
In chronic diseases and convulsive disorders,rigor appears early and passes off quickly due to depletion of glycogen stores.In strychnine poisoning,rigor sets in almost immediately and passes off early.
In cases of sudden death,in healthy adults,a late onset and long duration is usual.
In death from drowning,rigor appears early due to muscular exhaustion but lasts longer due to coldness of water.
Rigor is frequently absent in septicemic conditions.
Surroundings effect:-Rigor is delayed by cold and accelerated by heat.
It should be differentiated from other causes of postmortem muscular stiffening or condition simulating rigor mortis such as:
a)Cadaveric spasm.
Cadaveric spasm OR Instantaneous rigor
It is the muscular stiffening in special muscles and special type of death.
* It occurs in voluntary muscles and in cases of deaths accompanied with violence (violent death).
*Accompanied by severe mental and nervous excitation.
-It occurs as a continuation of the antemortem contraction of muscles Justbefore death without passing the stage of primary flaccidity.
-Cadaveric spasm records the last act of life Justbefore death.
Cadaveric spasm cannot be fabricated.
-Cadaveric spasm occurs in injuries of the CNS, drowning, suicide, struggling homicide and such cases of death with nervous over stimulation.
Medicolegal importance
of
cadaveric spasm
1-In cases of drowning, the dead animal keeps the mouth grasping some aquatic plants, weeds, and mud which is a sure sign of drowning.
2-In human forensic medicine, the hand of the victim is seen firmly grasping the weapon in suicide or the cloths or hairs of the assailant in homicide.
When a group of muscles of a dead body were in
state of strong contraction immediately prior to
death and remain so even after death, the condition
is termed as – (AIIMS May 05)
a) Gas stiffening b) Rigor mortis
c) Cadaveric spasm d) Cold stiffening
b)Cold stiffening.
Cold stiffening of muscles is due to the effect of very low temperature or freezing. It is reversible if the dead body warmed, the dead body then passes the primary flaccidity and rigor mortis as soon as thawing takes place.
c)Heat stiffening.Exposure of a body to intense heat results in heat stiffening due to coagulation of the muscle protein. Shortening of the muscles due to the effect of heat or fire of hot liquids. Heat coagulation or stiffening persists till the beginning of secondary flaccidity.
Cold stiffening may be associated with –
a) Trench foot (AIIMS 80, AMC 85)
b) Immersion foot
c) Body rigid, heavy and stiff
d) .Any of the above
It’s a POST-MORTEM finding
Rigor mortis is simulated by – (AIIMS 92)
a) Mummification b) Algor mortis
c) Cadaveric spasm d) All of the above
Rigor moreis in a foetus develops after
attaining – (TN 02)
a) 3 months of age b) 4 months of age
c) 7 months of age d) 10 months of age
Rigor mortis develops …. after death-(PGI 86,87)
a) 1/2- 1 hr. b) 1 to 2 hrs
c) 3 to 6 hrs. d) 12 hrs.
Rigor mortis first starts in – (PGI 81, AIIMS82)
a) Upper eyelids b) Lower eyelids
c) Lower limbs d) Fingers
Prolongation of Rigor mortis is seen in – (PGI 03)
a) Lead b) Arsenic
c) Mercury d) Copper
Delayed rigor mortis occurs with – (UP 07)
a) Vegetables poisons b) Strychnine
c) Opium d) Septicemia
Pugilistic attitude is due to – (PGI 99)
a) Coagulation of proteins b) Cadaveric spasm
c) Rigor mortis d) Coagulation of fats
Seen in heat stiffening






![clip_image003[4] clip_image003[4]](https://criticalcaremcqs.com/wp-content/uploads/2011/01/clip_image0034_thumb.jpg?w=547&h=286)
![clip_image005[4] clip_image005[4]](https://criticalcaremcqs.com/wp-content/uploads/2011/01/clip_image0054_thumb.jpg?w=576&h=301)





























































































